WASHINGTON — With two full-time jobs and watching his two kids full-time, Ali Popal has his hands full. The 37-year-old realtor, engineer and parent, is trying to do it all.
But before he can do anything he needs to keep his glucose in check.
“I'm a type one diabetic—I'm insulin-dependent," Popal said. "So my pancreas does not produce any insulin.”
For more than three decades he's relied on insulin to balance his blood sugar levels. Without it, he can go into Diabetic ketoacidosis or DKA. He has before.
In some cases, DKA could lead to a coma.
"It's like oxygen," Popal said.


Right now he pays under $50 for five vials of insulin, but back in 2008 when he was unemployed and uninsured, he said he paid between $400-$800 a month.
"Why does it cost so much?" Popal asked.
This is the question lawmakers around the country, from both parties, are asking. That includes President Biden, who has been pushing for legislation that would cap insulin copayments at $35. During his State of the Union address in February, he offered this critique of the drug companies.
“Insulin costs about $10 a vial to make, that’s what it costs the — the pharmaceutical company," Biden said, "But drug companies charge families...up to 30 times that amount.”


The President has since doubled down on this claim that insulin costs dollars to make but is sold for hundreds.
To get context on this complicated issue, our Verify researchers spoke with Dr. Gerard Anderson, a health policy and management professor at Johns Hopkins, and Dr. Robert Lash, chief medical officer at the Endocrine Society.
We also read a U.S. House Oversight and Reform Committee report on drug pricing and watched a 2019 Congressional hearing.
Anderson and Lash agreed that $10-$25 is a fair estimate of the cost to create insulin.
Dr. Lash referenced a 2018 study that found that a vial of insulin could be made for the low costs of $3-$8.
"So you could put that at kind of the low end, and then if you wanted to try to set a high end...there are some insulins that are available from Walmart and from CVS that are $25 a vial," Dr. Lash said. "I think it's safe to assume that the actual cost to produce a vial of insulin is somewhere between that lowest unit of $3-$8 a vial, and the lowest price you could possibly buy a vial of insulin for, which is $25."
Why is insulin so expensive?
As for the price of insulin, that's complicated.
"It's a huge market with only three manufacturers,” Anderson said.
In fact, according to Anderson and the House Committee report, just three drug companies make up 90% of the global insulin market.
Here are the approximate list prices for a 10mL vial of insulin according to the report:
- $275 for Humalog made by Eli Lilly
- $284 for Lantus made by Sanofi
- $290 for Novolog made by Novo Nordisk
“There's three manufacturers and they keep raising the prices, they've been raising the prices for the past 20 years," Anderson said.
In 1996 Humalog's subcutaneous solution cost $20.82. That means today's price tag is approximately 1219% higher than when it debuted 26 years ago.
It's the same story for Lantus, which cost $34.81 in 2001—now roughly 715% higher; and NovoLog, which cost $39.75 in 2001— now roughly 628% higher.
But these list prices, set by the manufacturer, are just the first piece of the puzzle. Insurance companies will then negotiate a lower price through Pharmaceutical Benefit Managers, or "PMBs."
The big three are CVS Caremark, Express Scripts and OptumRx.
The PBMs play a crucial role. Our experts say they decide which drugs get a favorable placement on what’s called a "formulary." It's essentially the list of drugs your insurance will cover. So making these PBMs happy with big rebates is a huge deal for pharmaceutical companies.
“As time has gone on the rebates have gotten larger, and in response, the drug companies have been charging more for their insulin, so they can afford to give the rebate to the insurance companies," Lash said. "So there's been this dance where the rebate goes up, the price goes up, the rebate goes up, the price goes up.”
And if you have good insurance — this dance may not impact you much, since you'll only see that reduced price.
Who ends up paying the list price?
But it's a different story for those with a high deductible.
"Until they've incurred three, five, 10 thousand dollars – they're going to have to pay the list price – unless their insurance somehow is negotiated something for them. But that's not common," Anderson said.
It's a worst-case scenario for those without coverage.
“If you don't have insurance at all, you're going to be paying list price – that $300 a vial," Lash said.
It's the same situation for Medicare patients who don't opt into Medicare Part D, the prescription plan.
"If you are a Medicare beneficiary you do not have to buy Part D coverage, the drug benefit, and so there could be Medicare beneficiaries without the drug benefit that would end up paying list price," Anderson said.
Response from the big insulin companies
Our team reached out to the three pharmaceutical companies and listened to their 2019 testimony.
They essentially argued the list price is a red herring because it doesn’t factor in the big rebates. They say people should focus on that price, the "net price," instead.
"Despite rhetoric about skyrocketing insulin prices, the net price (meaning the amount that Sanofi actually receives from a sale of its medicine after payment of any rebates or discounts on such sale) of insulin has been falling for seven consecutive years, making our insulins significantly less expensive for insurance companies," a Sanofi statement reads in part.
It continued: "PBMs have demanded rebates for pharmaceutical products for nearly two decades, and they are an ingrained feature of our healthcare system. Since 2012, the net price of our insulins declined by 54%. Over the same period, the net price for commercial and Medicare Part D plans of our most prescribed insulin, Lantus, has fallen 62%, while average out-of-pocket costs for patients with commercial insurance and Medicare has risen approximately 60%."
A spokesperson for Eli Lilly sent a similar reply.
"Pharma manufacturers do not sell their medicines straight to consumers. There is a complex pharmaceutical distribution system that includes manufacturers, wholesalers, pharmacies, PBMs, and health plans who all contribute to the final cost that people with diabetes pay for insulin," an Eli Lilly statement reads in part.
It continued: "...It is also important to note that Lilly has not increased the list price of any insulin since 2017 and has taken numerous actions to help lower the average out-of-pocket monthly cost for a prescription of Lilly insulin by 44 percent over the last four years, to $21.80 – including new initiatives that ensure anyone is eligible to purchase their monthly prescription for $35, whether they are uninsured or use commercial insurance, Medicaid, or a participating Medicare Part D plan."
The companies also said they have discounts available for those with and without insurance. You have to apply for these discounts, and it’s up to the pharmaceutical company if you’re approved.
Novo Nordisk sent VERIFY this statement: "Novo Nordisk is committed to providing support so that no patient has to go without insulin because they can’t afford it. The system we currently have is very complicated – rebates, discounts, administrative fees, co-pays and deductibles all play a role in what people with diabetes pay out-of-pocket. We have several new programs designed to address the accessibility and affordability of the therapies that patients rely on to manage their diabetes. Information about all of Novo Nordisk’s affordability offerings can be found at NovoCare.com. We encourage anyone in need to contact us."
So we can verify for the uninsured, some Medicare patients, or people with a high deductible, the answer is yes; they would have to pay hundreds of dollars unless they get a discount.
There are some cheaper alternatives out there, including "generics" or "biosimilars" from those same big pharmaceutical companies.
For example, a biosimilar called "ReliOn" is $25 per vial available at places like Walmart. It's based on an older insulin formulation. Dr. Lash says you should talk to your doctor before switching.
"Civica" a non-profit pharmaceutical company announced plans to make three generic insulins, and pending FDA approval, expects the first one to be available "as soon as early 2024."
Are there laws trying to limit the price of insulin?
Lawmakers at the state and federal levels have been trying to come up with a solution to skyrocketing insulin prices for years.
The Affordable Insulin Now Act, which passed the House of Representatives 232-193, would cap monthly copays on insulin products at $35 or 25% of the plan's negotiated price for that drug (whichever is less). A similar bill, with slight variation pertaining to Medicare patients, was introduced in the Senate.

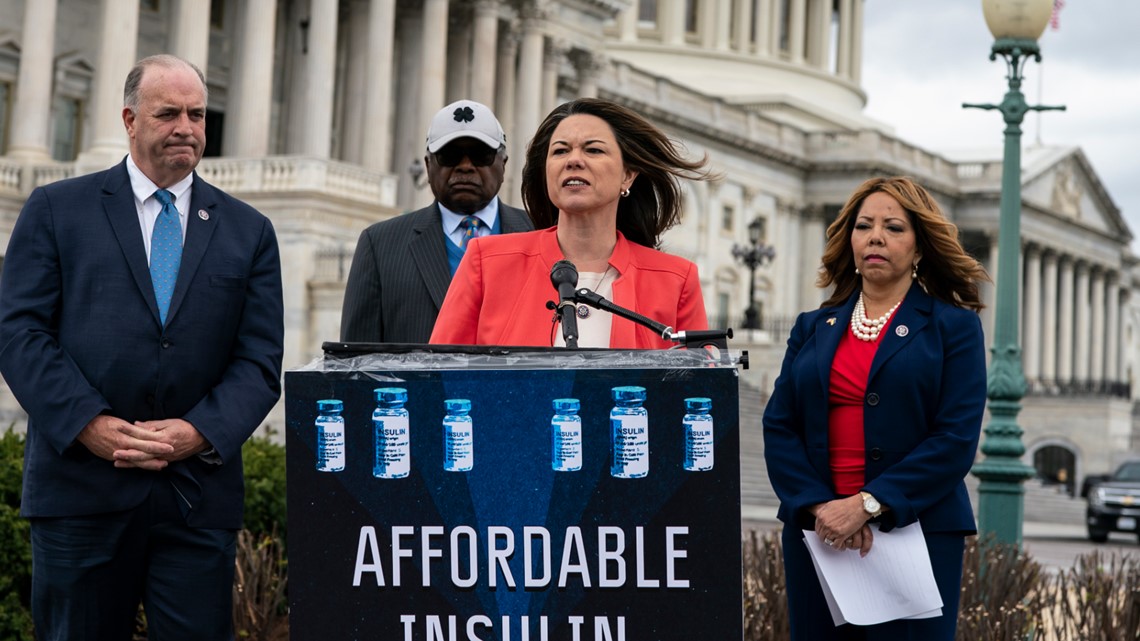
Several states have passed laws capping copayments, too.
Since January, D.C. started capping copayments at $30 a month; Virginia began capping copays at $50 for a 30-day supply at the beginning of 2021, and West Virginia has capped copay spending at $100, since 2020.
In Maryland, a similar bill that would limit copayments at $30 for a 30-day supply is awaiting the governor's signature. The governor could sign the bill, allow it to become law without signing it, or veto the bill entirely. A spokesperson for Governor Hogan's office said the bill is currently under review.
Delegate Joseline Pena-Melnyk, the bill's sponsor, told WUSA9 she expects the bill to go into law and take effect beginning Jan. 1, 2023.
WATCH: Verify reporter Evan Koslof speaks with Dr. Gerard Anderson to answer your questions about the cost of insulin.