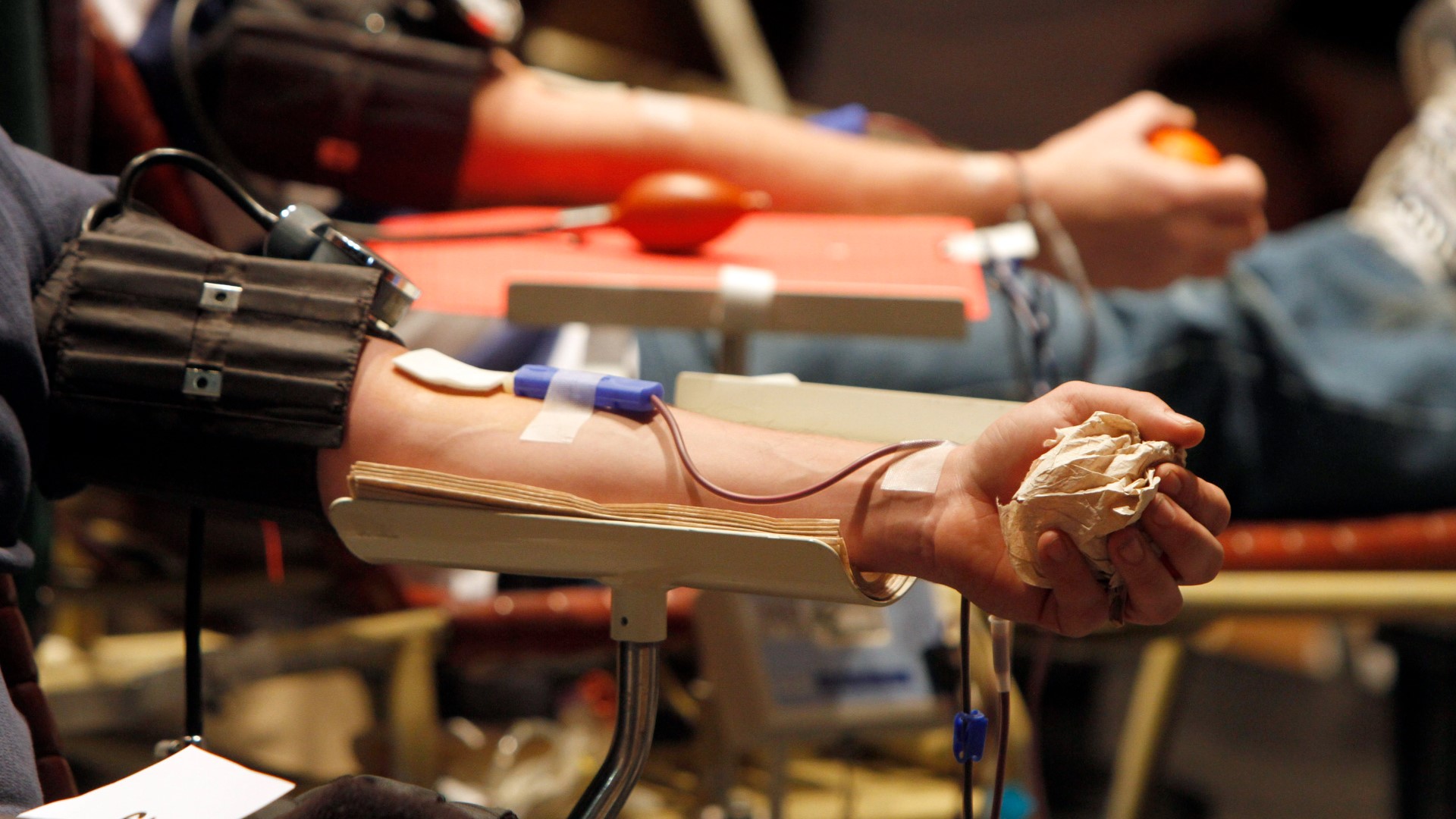
'We have the same blood as you' | Emerging study works to eliminate blood ban for gay, bisexual men
The ADVANCE Study aims to evaluate alternatives to the blood donor deferral policy for gay and bisexual men.

Since the rise of America's AIDS epidemic in the 80s, the FDA has banned men who have sex with men from donating blood. The rules have slightly been modified over time, but many believe the stipulations are biased. This is Episode 1 of a three-part series that explores the history of the blood ban, and the efforts to end it.
Blood Bias
For decades, gay and bisexual men have been banned from donating blood in some capacity, preventing them from contributing to alleviate blood shortages or helping a wounded friend.
"I think the ban has a history that becomes hard to discard," Dr. Melanie Thompson, co-chair of the HIV Medicine Association, said.
Medical experts have said it's a history tainted with bias, as the Food and Drug Administration (FDA) banned men who have sex with men from blood donation since the height of the AIDS epidemic.
"Back in the 80s, when the HIV crisis first broke, there was a lot of blood that was tainted with HIV," Dr. Claudia Cohn, chief medical officer of the Association for the Advancement of Blood & Biotherapies (AABB), said. "The risk at that time, in the early 80s, was somewhere around 1 in 100."
Cohn said that ratio has decreased exponentially, with the risk of contracting an infectious disease through blood now somewhere within the range of 1 in 2 million.
As research, treatments, testing and detection advance, new HIV infections reduced globally since its peak in 1997 by 52%, according to 2021 research from The Joint United Nations Programme on HIV/AIDS (UNAIDS).
People continued to die from HIV throughout the 80s with mortality peaking in 1995. A Kaiser Family Foundation study shows those rates have decreased by more than 80% in the last three decades.
"As we have learned more and more about HIV, as we have learned more and more about diagnostics to detect HIV, the science of blood donor screening hasn't kept up," Thompson said.
Now, decades since the initial ban was implemented, restrictions and celibacy requirements for gay and bisexual men still remain.
Emerging research
The FDA is currently funding new research that could eliminate the ban all together. It's called the ADVANCE Study, which stands for Assessing Donor Variability And New Concepts in Eligibility.
The study aims to evaluate alternatives to the blood donor deferral policy for gay and bisexual men by changing the questions blood donors are asked.
"Every time you're going to donate blood, you fill out a questionnaire," Josh Stowell said. "I would see that question on there."
The current questionnaire asks male donors if they have had sexual contact with another male.
"Basically it's called self-disqualification," Stowell said.
That questionnaire is what made Stowell and Ben Nicoara want to be first in line to participate in the study.
"I actually had no idea that there was a lifetime ban, like when I tried to go give blood one time," Nicoara explained.
From confusion to embarrassment, Nicoara and Stowell said there were many emotions surrounding their ability to donate blood.
"Having to just forcefully stop doing something that you really, really want to do is like, it was debilitating, honestly. You also kind of felt a little bit of shame because of your sexuality as well," Stowell said.
Now, medical and testing advancements allowed the FDA to reconsider an expansion to the blood supply.
A different approach
Dr. Cohn added that the chances of someone developing AIDS from a blood donation is slim to none.
"It would be easier for you to get struck with lightning than to contract AIDS through a blood transfusion," Cohn said.
She is advocating for a different approach.
"It makes a lot more sense if we went to what is called individual risk-based assessment, which takes a generalized approach. It doesn't ask what your gender is. It doesn't ask what your sexual preferences are. It simply assesses whether you are at greater risk based on your sexual history," Cohn explained.
The FDA said its working toward change, issuing a statement saying:
"The FDA remains committed to considering alternatives to time-based deferral by helping to generate the scientific evidence that is intended to support an individual risk assessment-based blood donor questionnaire."
But Cohn believes it will be a while before we see that shift.
"FDA is all about the safest blood possible," she said. "They need to study this question extensively before they will change their policy."
The ADVANCE Study needs 2,000 participants across eight cities — Atlanta being one of them. Once it's complete, the FDA will study the data again before making any alterations to the questionnaire.
"I would just hope that men who have sex with men would be treated the same as anybody else. It's like, we're not we're not less than. We have the same blood as you. The 'H' in HIV stands for human. It doesn't stand for anything else, so. It affects all of us," Nicoara said.
Blood Bias | Watch the full series
Episode 1: 'We have the same blood as you' | Emerging study works to eliminate blood ban for gay, bisexual men